Benefits of Research and Evidence-Based Practice in Exercise Science
This is an excerpt from Introduction to Exercise Science With HKPropel Access by Duane V Knudson.
By James Farnsworth and Natalie Myers
Many exercise and sport science professionals conduct research because they want to help clients and positively affect practice in their field. Researchers also are inquisitive by nature and like to find answers to questions. In this professional field it is particularly important “to address questions that have the potential to improve performance” (Bishop et al., 2006, p. 167). These questions about performance can be influential to other professionals such as coaches, athletes, and administrators. Research is a fantastic way to show proof of concept and outcomes that can be used to leverage decision making or even change outdated ways of thinking. Research in sports medicine and exercise science also focuses on questions about factors influencing risk of injury and the reduction of and treatment of injury.
Having a sound background in research methods and evaluating evidence allows you to bridge the gap between the controlled research environment and the messier and complex real-world environment of the clinic, field, and gym. Even if the act of conducting the actual research does not interest you, understanding where to search, how to search, and how to interpret and critically appraise exercise science research can improve professional practice and client interaction. The understanding of research also allows you to engage in evidence-based practice.
Key Point
Exercise science research generally focuses on two main benefits: improving performance and reducing risk of injury.
Evidence-Based Practice
Evidence-based medicine (EBM) is a phrase grounded in European philosophical mid-19th-century origins. A consistent definition of EBM did not arise in the scientific literature until the 1990s with the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients (Sackett et al., 1996). In the 1990s EBM most often was recognized in the context of medicine, yet professionals outside of medicine were beginning to embrace and implement an evidence-based approach to practice and learning. Consequently, Dawes and colleagues (2005) advocated for a transition from EBM to evidence-based practice (EBP) to encompass not only health care professionals, but all professionals adopting an evidence-based approach to professional practice. EBP is a problem-solving approach that integrates the best available research, professional experience, and client values into practice. The purpose of EBP is to promote collaborative and inquisitive thinking from the professional to ensure quality care and a positive and an effective impact on the client.
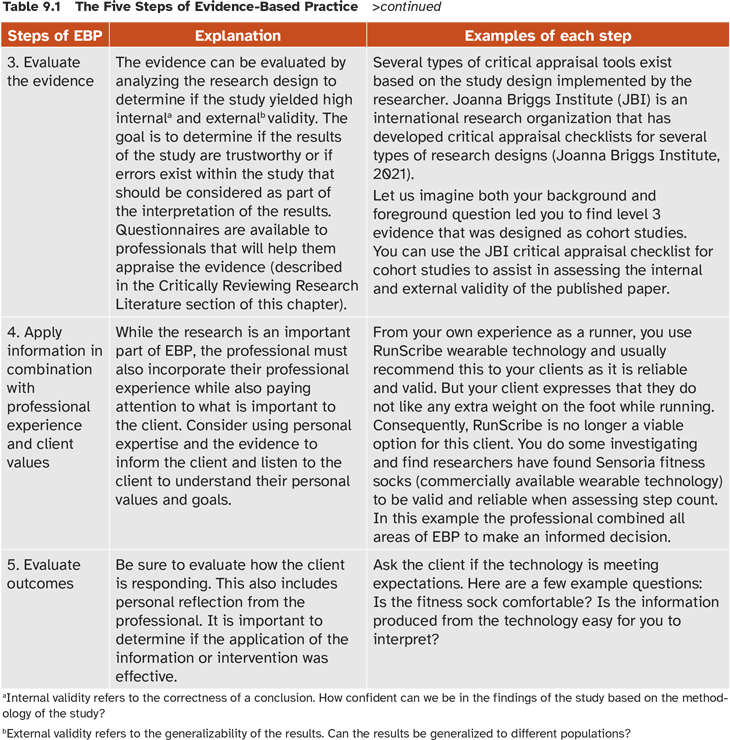
Researchers promoting EBP typically recommend a five-step process that allows for EBP implementation (Dawes et al., 2005; Johnson, 2008; Melnyk et al., 2011; Sackett et al., 2000). The details of each step of EBP are described in table 9.1.

Key Point
Evidence-based practice is a problem-solving approach that integrates the best available research, professional experience, and client values into practice. Integrating EBP into practice allows for well-informed decision making and the integration of the client into that decision-making process.
More Excerpts From Introduction to Exercise Science With HKPropel AccessSHOP

Get the latest insights with regular newsletters, plus periodic product information and special insider offers.
JOIN NOW
Latest Posts
- How do I integrate nutrition education into PE?
- How does the support of friends and family influence physical activity?
- What makes the Physical Best approach unique?
- Strength training gimmicks . . . or not?
- How do vitamins and minerals support our bodies?
- Why do many people have difficulty losing weight?


